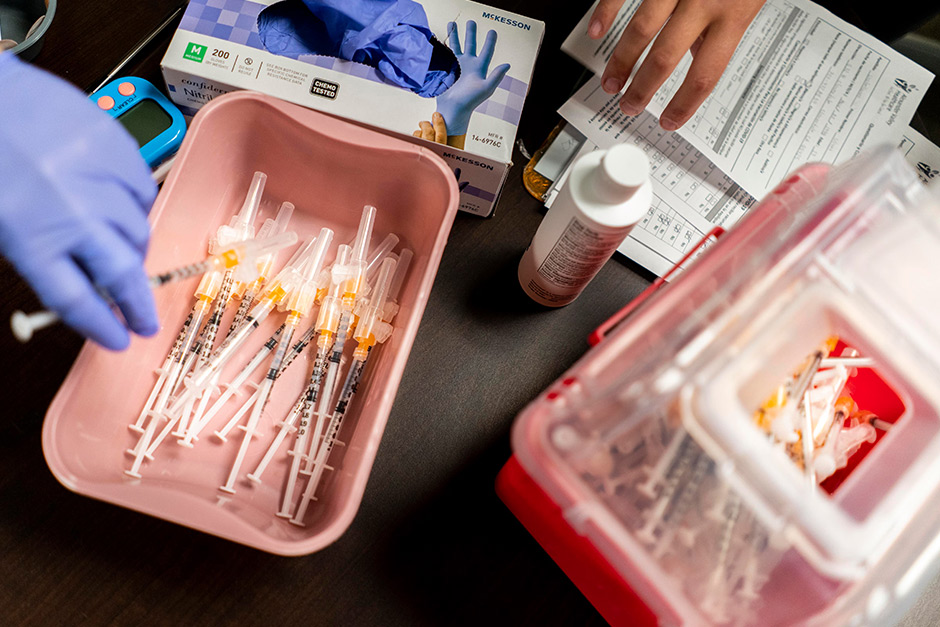
A significant tremor has rippled through the landscape of public health and regulatory oversight. The FDA, an institution long seen as the bastion of medical safety, is ushering in a new era of strict vaccine regulations. This pivot comes on the heels of a deeply concerning acknowledgment: their own findings suggesting tragic fatalities linked to child COVID shots. Such an admission isn’t merely a headline; it’s a foundational shift that demands our attention, reshaping not only policy but also the very trust we place in health authorities.
The Stated Catalyst: A Painful Acknowledgment
For any regulatory body to publicly acknowledge severe adverse outcomes, especially those as irreversible as death in pediatric populations, is a rare and solemn occasion. The FDA’s move to implement strict new vaccine rules is presented as a direct consequence of this internal evaluation concerning child COVID shots. This isn’t just about tweaking guidelines; it’s about a profound re-evaluation of past strategies and the data underpinning them. When an institution of this magnitude makes such a statement, it casts a long shadow, prompting urgent questions about the processes, oversight, and decision-making that led to previous recommendations.
The gravity of this situation cannot be overstated. For parents who made decisions based on previous assurances, this revelation is likely to be met with a complex mix of anger, grief, and a sense of betrayal. It forces a reckoning with the inherent risks in medical interventions, particularly for the most vulnerable among us. The new rules, whatever their specifics, must address not just future safety but also the mechanisms by which such tragic outcomes were understood, or perhaps, not adequately understood, in the past.
Rebuilding Trust and Reshaping Future Policy
The immediate aftermath of such an announcement is undoubtedly a crisis of confidence. Public trust, once eroded, is incredibly difficult to restore. The FDA’s challenge now extends beyond simply implementing stricter rules; it involves a monumental effort to be transparent, accountable, and proactive in demonstrating a renewed commitment to absolute safety. The coming regulations will likely focus on more rigorous pre-market testing, enhanced post-market surveillance, and perhaps a more conservative approach to emergency use authorizations, especially for children.
Beyond the immediate regulatory changes, this development ignites a broader conversation about medical ethics, informed consent, and the balance between public health urgency and individual safety. “This isn’t just about new regulations; it’s about deeply understanding past actions and ensuring accountability for future health strategies,” remarked a prominent public health ethicist, underscoring the critical need for introspection and structural improvements. The new rules must aim to prevent any recurrence of such devastating outcomes, ensuring that future interventions for children are approached with the utmost caution, backed by an irrefutable body of safety evidence.
The Path Forward: Vigilance and Informed Choice
As these strict new rules come into effect, the onus remains on both regulatory bodies and the public to engage with health information critically and thoughtfully. For families, this development underscores the vital importance of open dialogue with healthcare providers, asking pointed questions, and understanding the evolving landscape of medical guidance. For the FDA, this moment presents an opportunity, albeit a painful one, to redefine its commitment to public safety, learning from past oversights and setting a new, higher standard for vaccine development and approval, particularly for pediatric populations. The conversation is far from over; it has only just begun to truly address the profound implications of these findings.
*